
And it’s a really important process, that these are not experiences and thoughts that are alone in the child’s head, but that the parent and the child have a way of talking and communicating about these things. That you can then put these things away without all those negative thoughts about yourself.Īfter the trauma narrative is created (and it can be done in multiple ways - actually writing a story, or some children do it with cartoons or drawings), it’s something that’s shared with the caregiver. You make those links and then lots of times you can realize that the way you made sense of the horrible things that happened to you - it’s not because you were a bad person, it’s not because you deserved it, it’s not because you should have been able to stop it and you couldn’t have. But yet she had this sense of, “I’m really not worthwhile.” And so, taking out and examining what are the thoughts you have as to why things happened, is really - it’s called trauma-focused CBT because it does have cognitive behavior therapy elements, where you look at the cognitions and how that affects your emotions and how that affects your behaviors. And the reality is that there’s nothing that justifies a parent choking a child. I remember one adult saying to me she couldn’t remember what she did that made her father want to choke her. And it’s important that oftentimes when things have happened to you, how you make sense of it affects how you feel about yourself. If we just shove it in there, you can’t really close the suitcase. And by taking it out of the box and examining it, it allows us to pack it up and really put it away. One of the core symptoms of PTSD is avoidance, and there’s that sense of, “I’ll be fine if I just don’t think about it.” But the reality is, it comes back, and our experiences shape us. Once there’s a set of skills and feeling like some sense of mastery, then the next major component is the trauma narrative, which is basically a revisiting of the trauma: Telling the story, and also the cognitions and the thoughts that go along with it. What are some skills I can use that will help them manage those behaviors and not have things escalate? And the training and skills the parent wants are, how do I manage the child when they get irritable or they may be oppositional or they don’t want to sleep. 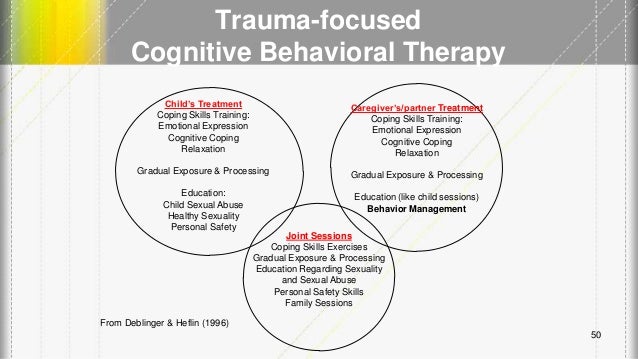
Being able to develop a sense of skills to deal with extreme anxiety: Relaxation training, thought-stopping techniques for recurrent memories. So psychoeducation is the first component. So starting to get a catalog of what are those things that elicit these symptoms helps you begin to get control of it. Running into a perpetrator is often going to elicit extreme anxiety and might also elicit irritability. 
So if a child has been exposed to domestic violence, yelling can be a trigger. And it also helps the parent make sense of what the kid is experiencing, and understanding that trauma triggers often elicit some negative behaviors. And to understand that these are all part of a syndrome, and common experiences for people who have been through the type of things that you went through, in and of itself is therapeutic. For individuals with a history of trauma who might meet criteria for post-traumatic stress disorder, it can be a very unnerving experience. You frequently have flashbacks, you may hear the perpetrator’s voice, you have trouble sleeping, trouble concentrating, you may feel cranky and irritable. The first thing is both the parent and the child need to learn what are normal trauma responses. The first component is psychoeducation, and it involves both the parent and the child. Trauma-focused CBT is the treatment that’s been developed for children with post-traumatic stress disorder that has the strongest evidence base to date.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
